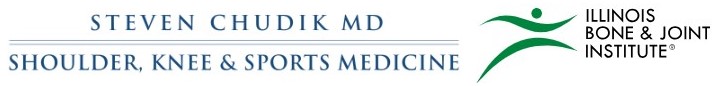Proper warm-up, conditioning exercises can help prevent youth sports injuries
Proper warm-up, conditioning exercises can help prevent youth sports injuries
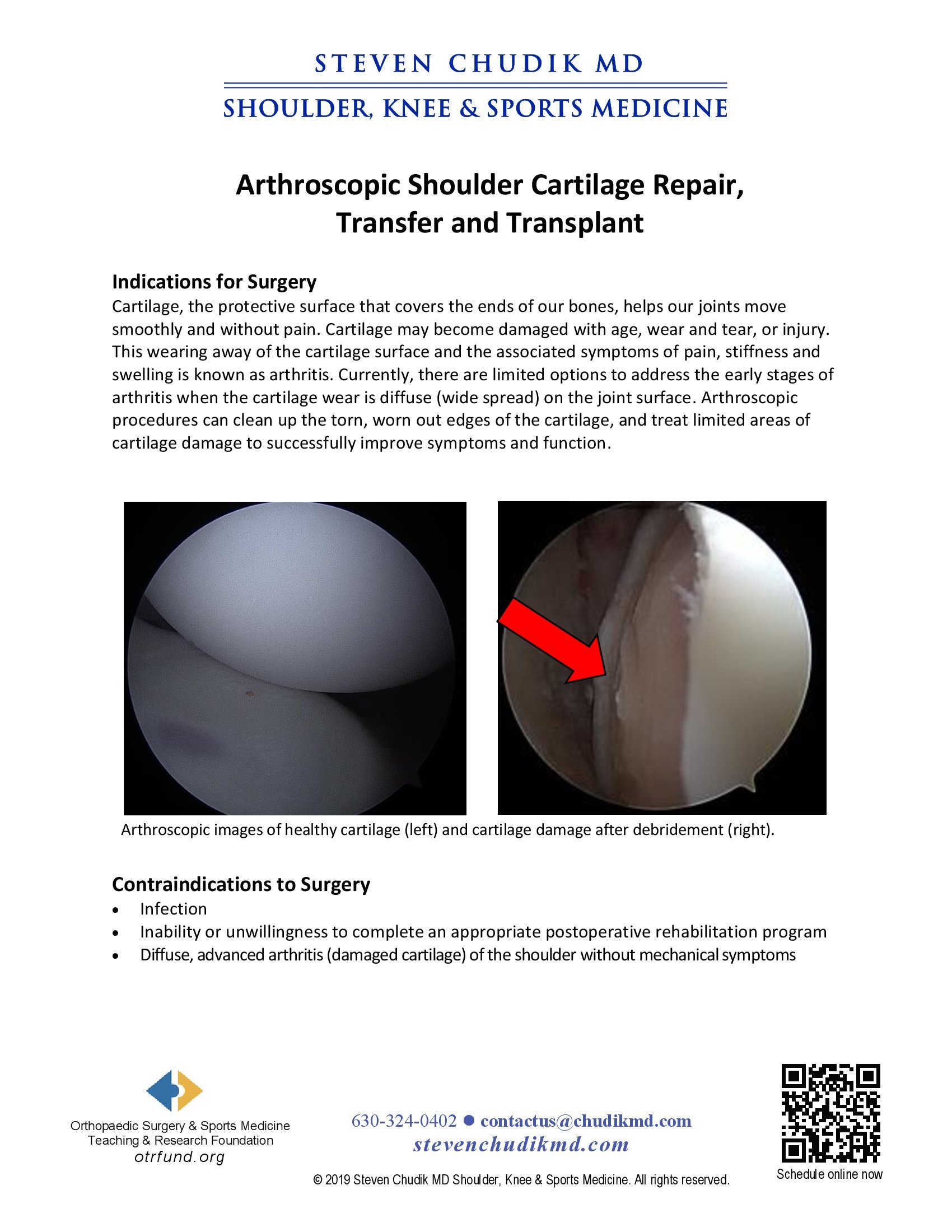
Cartilage, the protective surface that covers the ends of our bones, helps our joints move smoothly and without pain. Cartilage may become damaged with age, wear and tear, or injury. This wearing away of the cartilage surface and the associated symptoms of pain, stiffness and swelling is known as arthritis. Currently, there are limited options to address the early stages of arthritis when the cartilage wear is diffuse (wide spread) on the joint surface. Arthroscopic procedures can clean up the torn, worn out edges of the cartilage, and treat limited areas of cartilage damage to successfully improve symptoms and function.
Learn More
 Santi simultaneously rebuilds his shoulder and his house
Santi simultaneously rebuilds his shoulder and his house
Dr Steven Chudik founded OTRF in 2007 to keep people active and healthy through unbiased education and research. Click to learn about OTRF’s free programs, educational opportunities and ways to participate with the nonprofit foundation.
1010 Executive Ct, Suite 250
Westmont, Illinois 60559
Phone: 630-324-0402
Fax: 630-920-2382
(New Patients)
550 W Ogden Ave
Hinsdale, IL 60521
Phone: 630-323-6116
Fax: 630-920-2382
4700 Gilbert Ave, Suite 51
Western Springs, Illinois 60558
Phone: 630-324-0402
Fax: 630-920-2382

© 2025 © 2019 Copyright Steven Chudik MD, All Rights Reserved.